Overview
Barton Surgery had already introduced care navigation, but it was not being used consistently across the team. This created variation in how patients were assessed and where they were directed.
Working with Xytal, the practice took a structured, team led approach to rebuilding care navigation from the ground up. The focus was on consistency, confidence and making the process work in day to day practice.
The result was a more reliable care navigation model, improved access, better use of clinical time and a team that felt confident in how they supported patients.
The challenge
At the start of this support period, care navigation was in place, but it was not working as intended.
The framework was not being completed consistently, and some team members had returned to previous habits, booking GP appointments without fully exploring patient need or alternative services.
There was no structured observation, no feedback loop and no clear data to show whether care navigation was being done well.
This led to several issues:
- Avoidable GP and nurse appointments
- Inconsistent information for patients
- Informal signposting with no data capture
- A lack of confidence within the team, particularly when patients challenged redirection
The practice knew it wanted to improve, but did not have a clear way to identify gaps or track progress.
The approach
Xytal worked alongside the practice to rebuild care navigation in a way that felt practical, consistent and owned by the team.
Rather than introducing a completely new model, the approach focused on strengthening what was already in place through a structured and iterative process, making changes step by step and learning as they went.
Listening first
Xytal facilitated a team workshop to create space for honest discussion about what was getting in the way. Three clear themes emerged:
- Time pressure and competition for appointments
- Lack of confidence in signposting
- Uncertainty about what good looked like
These were treated as practical challenges to solve, rather than individual performance issues.
Redesigning the process
A revised care navigation SOP was co-designed, incorporating the team’s feedback. This included a minimum standard for every contact (presenting complaint, duration, previous actions, patient’s outcome preference, red flag screening) and a workflow adjustment so team members could view appointment availability without leaving the template, removing a key frustration that had been driving early booking.
Building confidence
Xytal supported the practice to bring clinical backing into the process. A GP partner explained how the information recorded by care navigators supported clinical decision making.
This shifted perception, the template was no longer seen as a tick box task, but as a practical part of patient care.
A clear escalation route to a duty clinician was also introduced, giving staff confidence when they were unsure how to proceed.
“I was worried about the observations at first… it’s not scary at all now.”
Introducing observation and feedback
One to one observation sessions were introduced using a structured checklist. These were positioned as supportive and developmental.
The first round created some anxiety, so the approach was paused, reset and then reintroduced more carefully. Over time, confidence grew and staff began to actively engage with the process.
Using data to make signposting visible
Xytal worked with the practice to ensure signposting activity was coded and tracked, allowing it to be reviewed regularly.
This helped shift the conversation from assumption to evidence. Weekly discussions focused on what was happening and where further improvement was needed.
Creating a self improving system
A key part of the work was helping the practice build feedback loops into the process.
- Observations informed updates to the SOP
- Survey results shaped changes to training and tools
- Data was reviewed regularly and used to guide next steps
Over time, the approach became embedded and continued to evolve as part of day to day practice.
Working with Xytal
Xytal worked alongside Barton Surgery as an extension of the team, supporting both the practical changes and how those changes were embedded day to day.
This included:
- Facilitating team workshops to surface barriers and build a shared understanding of what needed to change
- Supporting the co design of a clear, workable care navigation SOP
- Introducing structured observation and feedback in a way that felt safe and developmental
- Helping the team use data more effectively, from signposting activity to access measures
- Bringing clinical and operational perspectives together to strengthen confidence in care navigation decisions
- Supporting the practice to build feedback loops so improvements could continue beyond the programme
The focus was not on introducing a new model, but on helping the practice make what they already had work consistently and effectively in practice.
The results
The work demonstrated that a consistent, human centred care navigation model can deliver measurable improvements without moving to total triage.
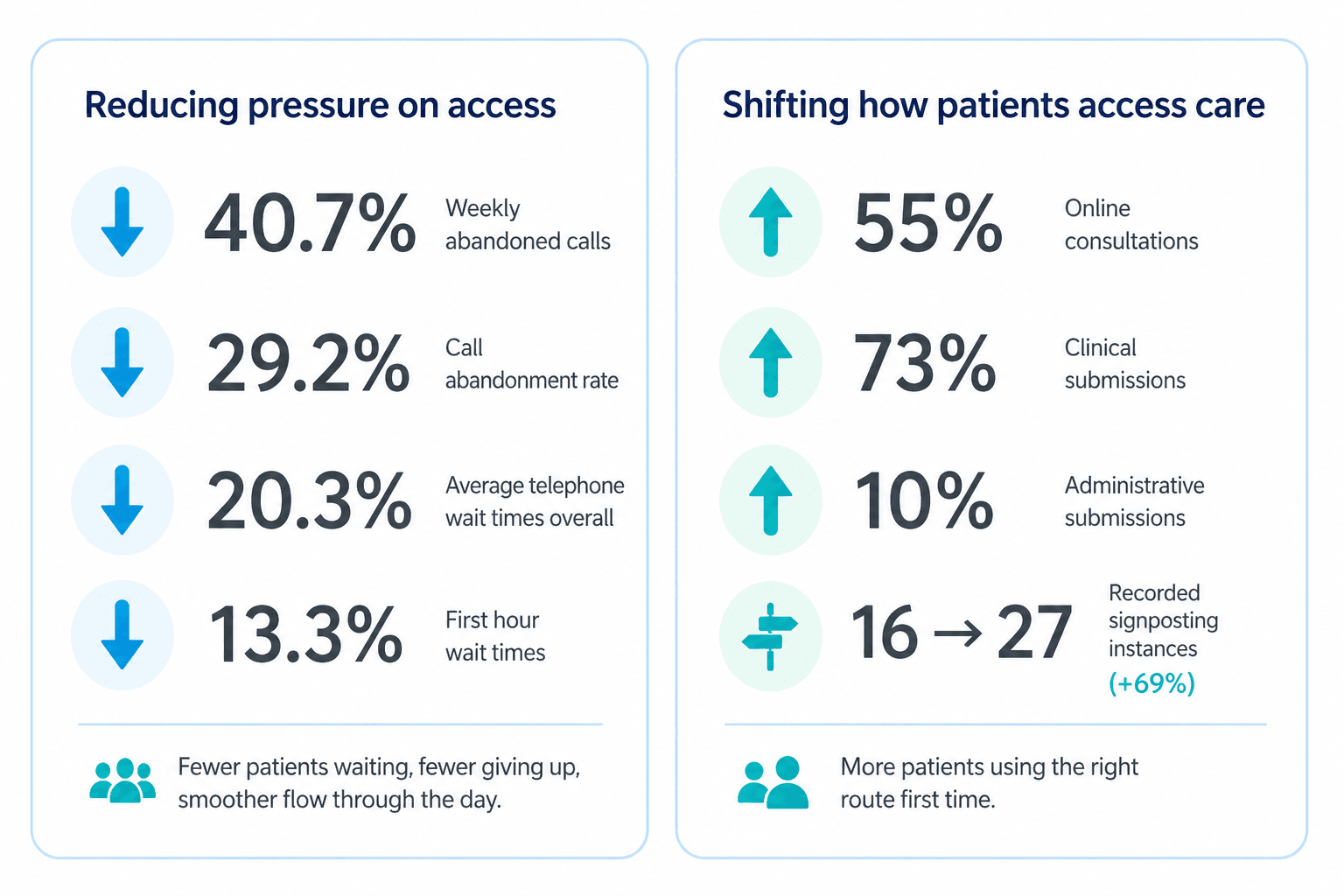
Staff experience
- The team moved from initial anxiety to actively engaging with observation and feedback
- Staff recognised the value of the template in supporting consistency and clinical decision making
- Confidence increased, particularly when redirecting patients to non GP services
- The practice was able to provide data to support system level conversations, including patient flow to urgent treatment centres
- The team demonstrated clear understanding of escalation routes and safety processes during inspection
- The model was shared confidently with peers, supported by evidence of both safety and outcomes
“The team now say ‘let me navigate you through this’… that shift in language tells you everything.”
What this meant in practice
Care navigation became consistent, visible and trusted, patients were more likely to be directed to the right service first time, clinical time was used more appropriately, and the team had a shared understanding of what good looked like.
“We never thought we would get to this point… the team now approach care navigation with real ownership.”
The work showed that a structured, team owned approach can deliver both safety and efficiency.










