Some of us (patients included) may not be aware that Radiology provides critical diagnostic and treatment services, with over 120,000 examinations a day across England. Clinical diagnosis is relying more and more on imaging to understand what is wrong with patients, with Radiology now featuring in four out of every five patient pathways, this has led to an increase in demand for imaging and led to rising pressures on Radiology departments. Demand for Radiology has increased rapidly over the past 20 years and is rising faster than that for NHS services as a whole, with advances in treatment and imaging, which improve diagnosis and treatments, also contributing to increased demand.
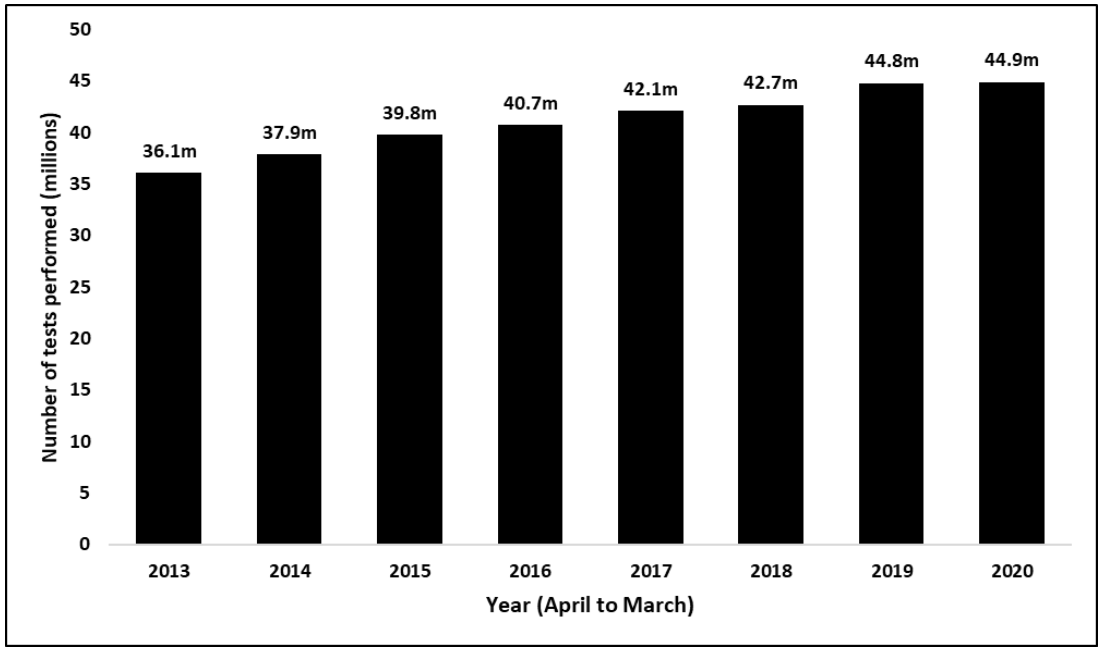
In the last two years, Covid-19 has also forced rapid changes in how departments operate, and this has added to an already overwhelming workload. In the initial phase of Covid-19, hospital attendance fell markedly with a fall in activity for most imaging modalities. Radiology Departments are now facing a backlog of imaging requests and are struggling to manage referral rates and waiting lists. There was a significant increase in the number of patients waiting over 6 weeks in September 2020. In May 2021, as part of the recovery of elective care, NHS England asked Radiology Departments to check and prioritise their waiting lists so that services could better understand the number of patients waiting and to inform service planning.
It may be obvious but it’s worth stating that these increased pressures also have a detrimental impact on the quality of patient care and staff morale. Radiology waiting times and report turnaround times have increased, which leads to increases in the time it takes for a diagnosis to be given by GPs and referrers, which means longer waits for treatment and longer stays in the hospital. These delays increase costs for departments, and ultimately the taxpayer, and have consequences for patients and departments in terms of patient wellbeing and outcomes.
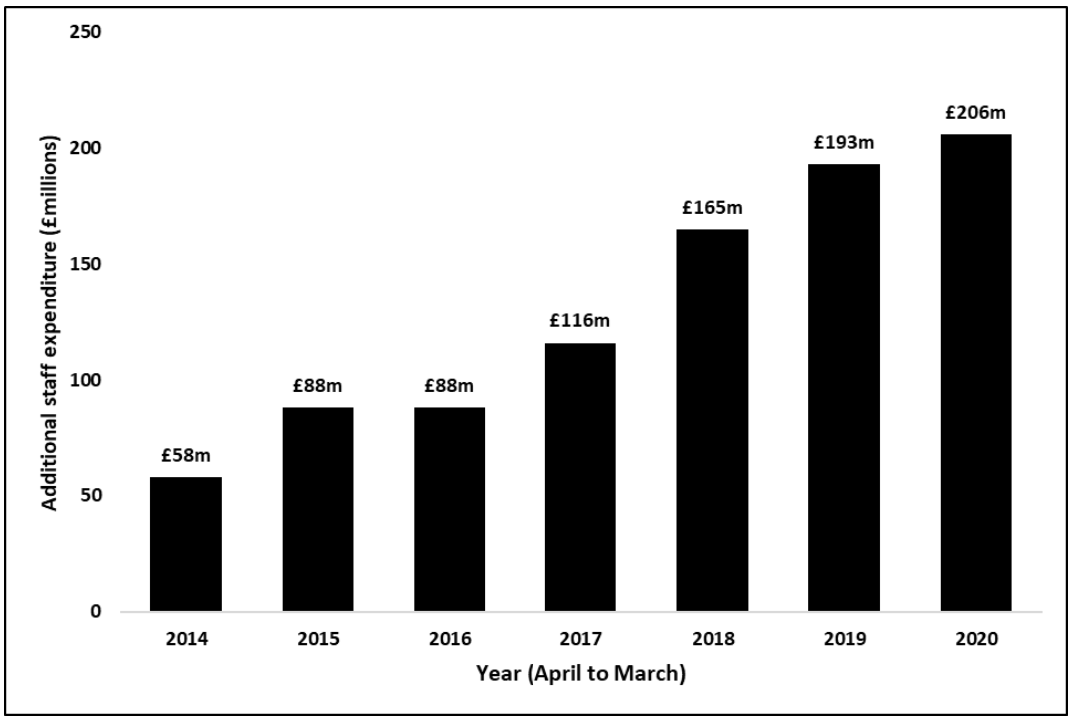
To add to this storm, Radiology is facing significant workforce shortages, which restrict departments’ ability to deliver care and has an impact on staff morale. In 2020, £206 million was spent on additional staffing capacity to try and meet demand, more than triple the spend in 2014, however this spending is a short-term solution, which may be making the problem worse, as it may draw staff out of permanent NHS roles in favour of outsourcing positions with better pay and conditions. This increases financial pressure on services and creates an unsustainable downward spiral (see Fig. 2).
With the issues we’ve described above, it is no wonder that the workforce is struggling, the RCR reports that staff have felt overwhelmed, undervalued, and burnt out for a long time. Covid-19 has also increased the pressure, with 92% of Trusts stating that they have concerns about stress and burnout among their staff due to the pandemic.
Recent reports have recommended setting up Imaging Networks which offers considerable opportunities to work at a larger scale to address workforce and capacity and demand challenges. They also offer the opportunity to review and improve clinical pathways and patient flow and to design new flexible ways of working at local and network levels. However, Imaging Networks also require strategic and operational leadership and staffing when Radiology Departments are already stretched, and the expectation is that this leadership and staffing will come from the existing workforce.
Xytal believes that by supporting Radiology to develop improvement capability, capacity, and confidence, at departmental and network levels our Radiology colleagues can address these complex, whole system pressures and challenges to create sustainable and resilient services now and in the future.
To see more of our work in Radiology, why not have a look at our Radiology Support Programme? Please don’t hesitate to Contact us to find out more, we’re always eager to assist you!
This blog was written by Elizabeth Dunn.
